Case Study
Collabor8
Hubio Technology
Overview
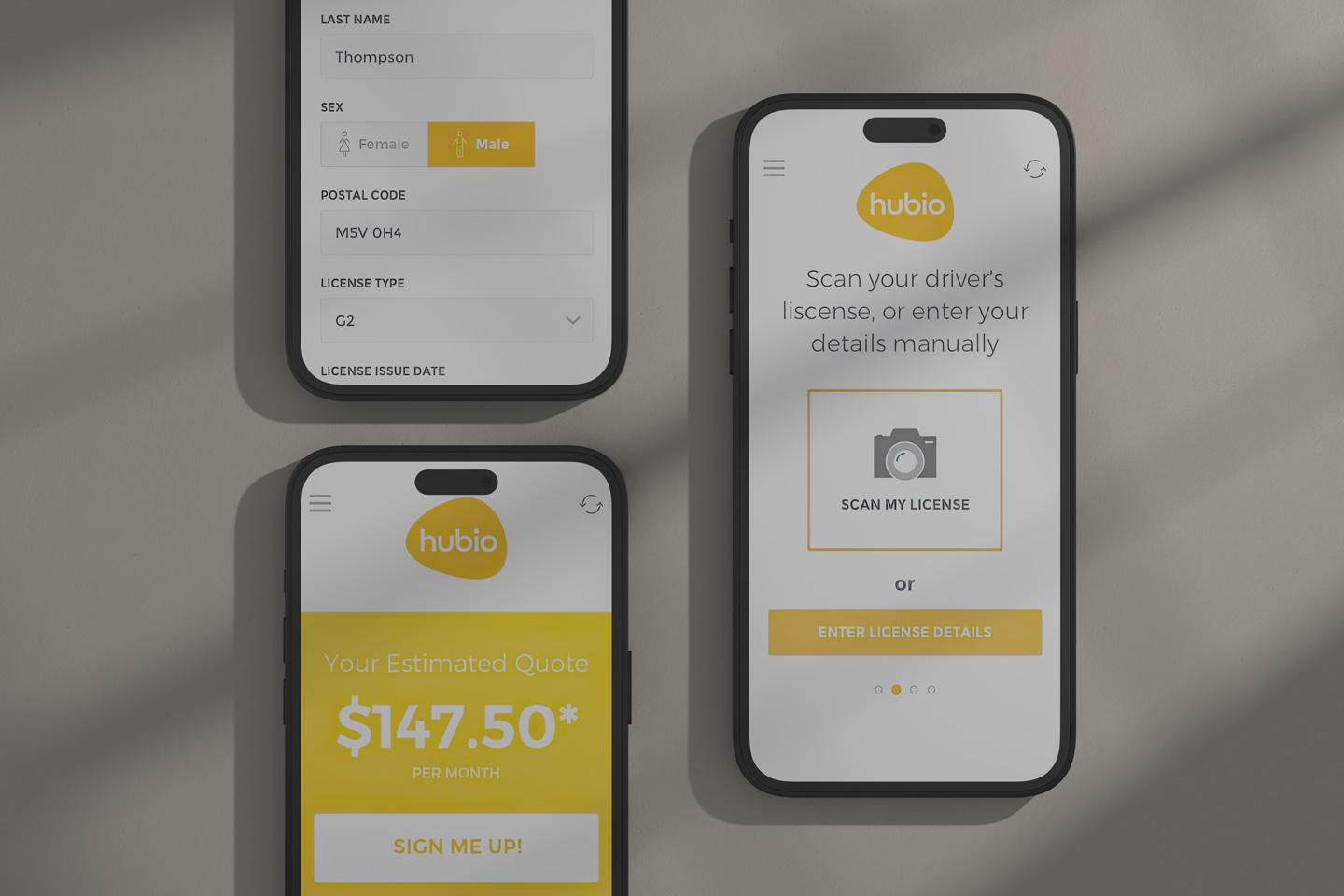
HUBIO Collabor8 is a SaaS platform designed to facilitate seamless integration for Property and Casualty insurance companies with various industry third-parties. Its goal is to provide reliable connectivity, automate insurance workflows, and streamline underwriting processes.
My Role
Customer Experience
User Experience
UI Design
Content Design
Identification of Problem
The primary challenge was to simplify and automate the communication and data integration between insurance company systems and third-party data providers, ensuring reliable and efficient workflows.
User Needs and Goals
The design was guided by the need for a system that could support various API formats, integrate third-party insurance data, and ensure security and compliance with North American standards.
User Research

Interviews
Conducted one-on-one interviews with insurance professionals and third-party agents using Hubio’s solutions. These discussions offered insights into how users interact with Hubio’s platforms, highlighting specific operational challenges and desired enhancements.
Personas
Created detailed personas for key user groups such as insurance agents, brokers, and regulatory bodies, derived from user interviews and market research. These personas helped in tailoring Hubio’s features to meet the diverse needs and expectations of its users.

Prototyping
Developed early prototypes of Hubio’s integration tools, including communic8. This allowed for practical demonstrations, enabling users and stakeholders to engage with the concepts, give feedback, and propose improvements directly relevant to their workflows.

Usability Testing
Performed extensive usability tests involving a variety of users from insurance companies to individual agents. These sessions were crucial in refining the user interface and functionality of Hubio’s platforms, ensuring they are intuitive and effectively meet the users’ needs.
Market Analysis
The need for a hub like communic8 was identified, considering its ability to support REST, SOAP, FTP, Message queue, and Spark API formats, and to provide vital integrations for the insurance sector.
Design Ideation
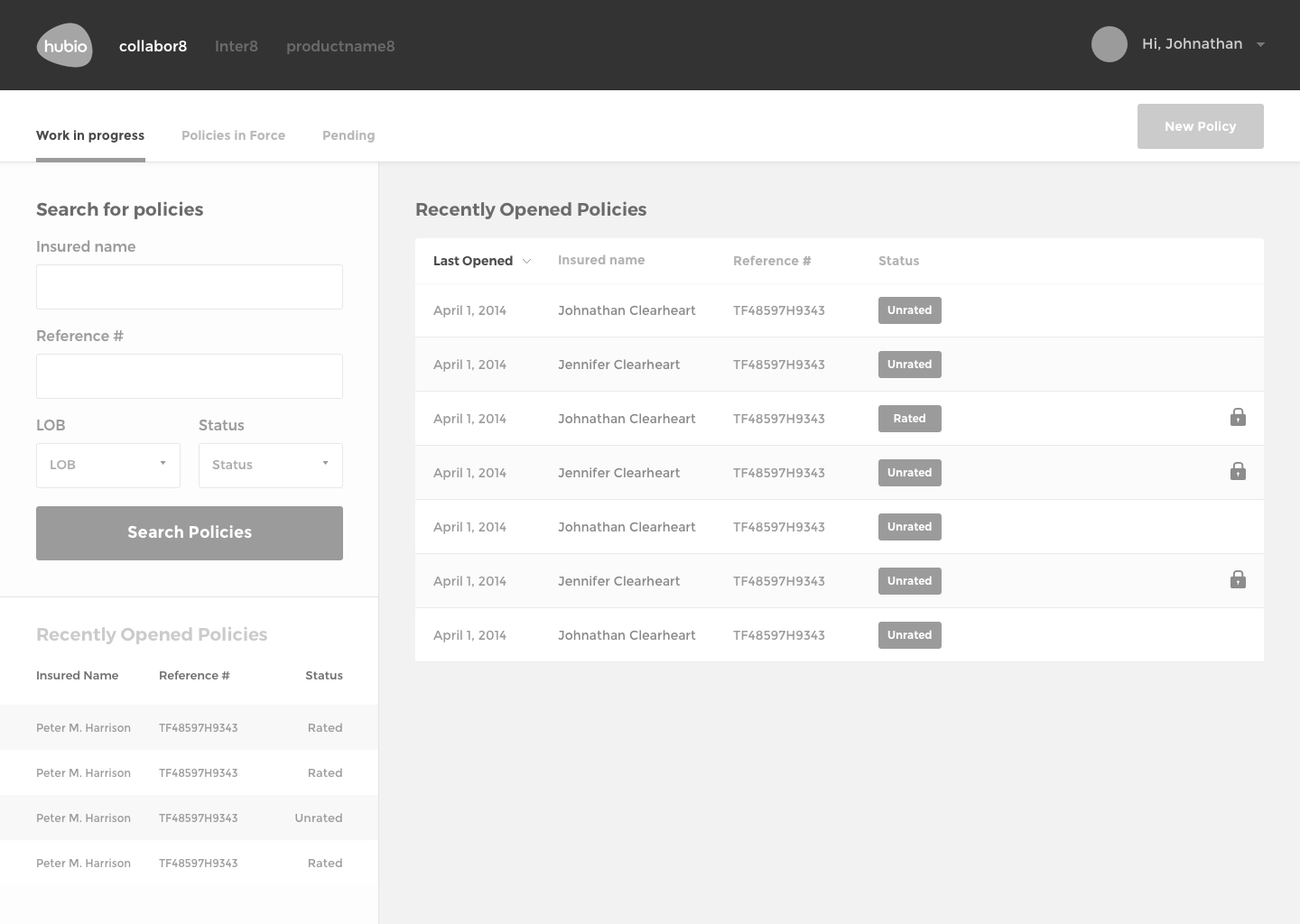
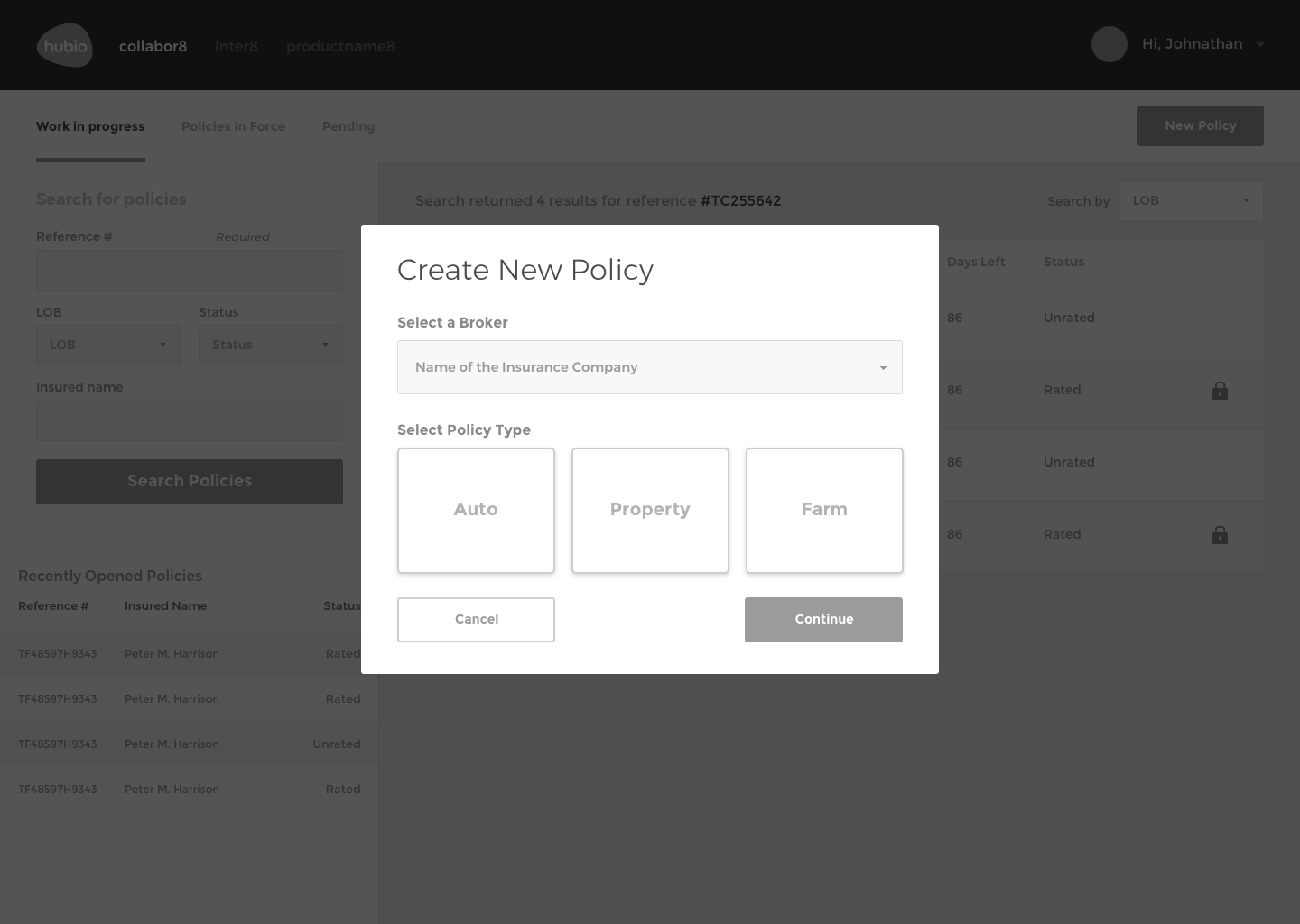
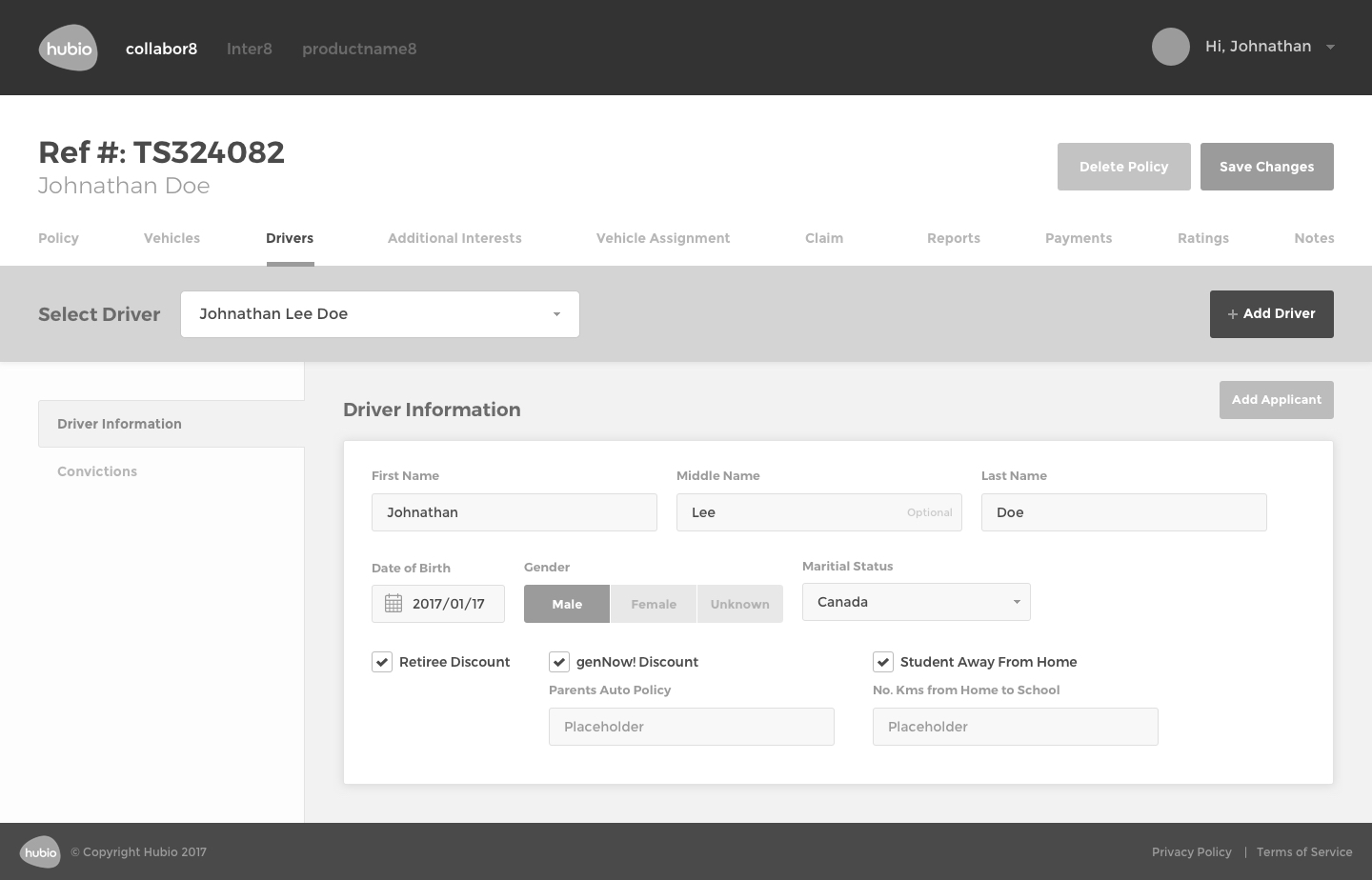
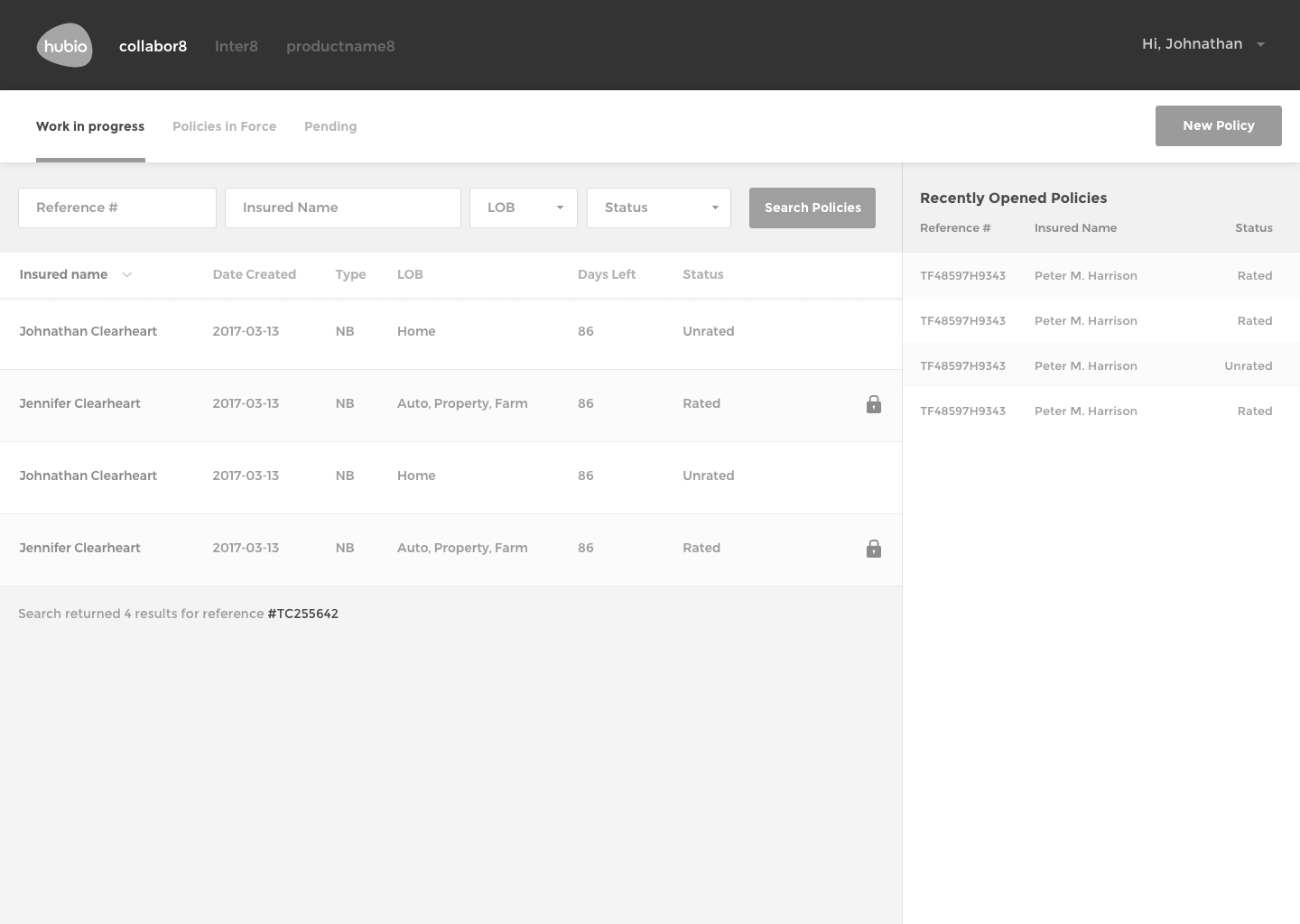
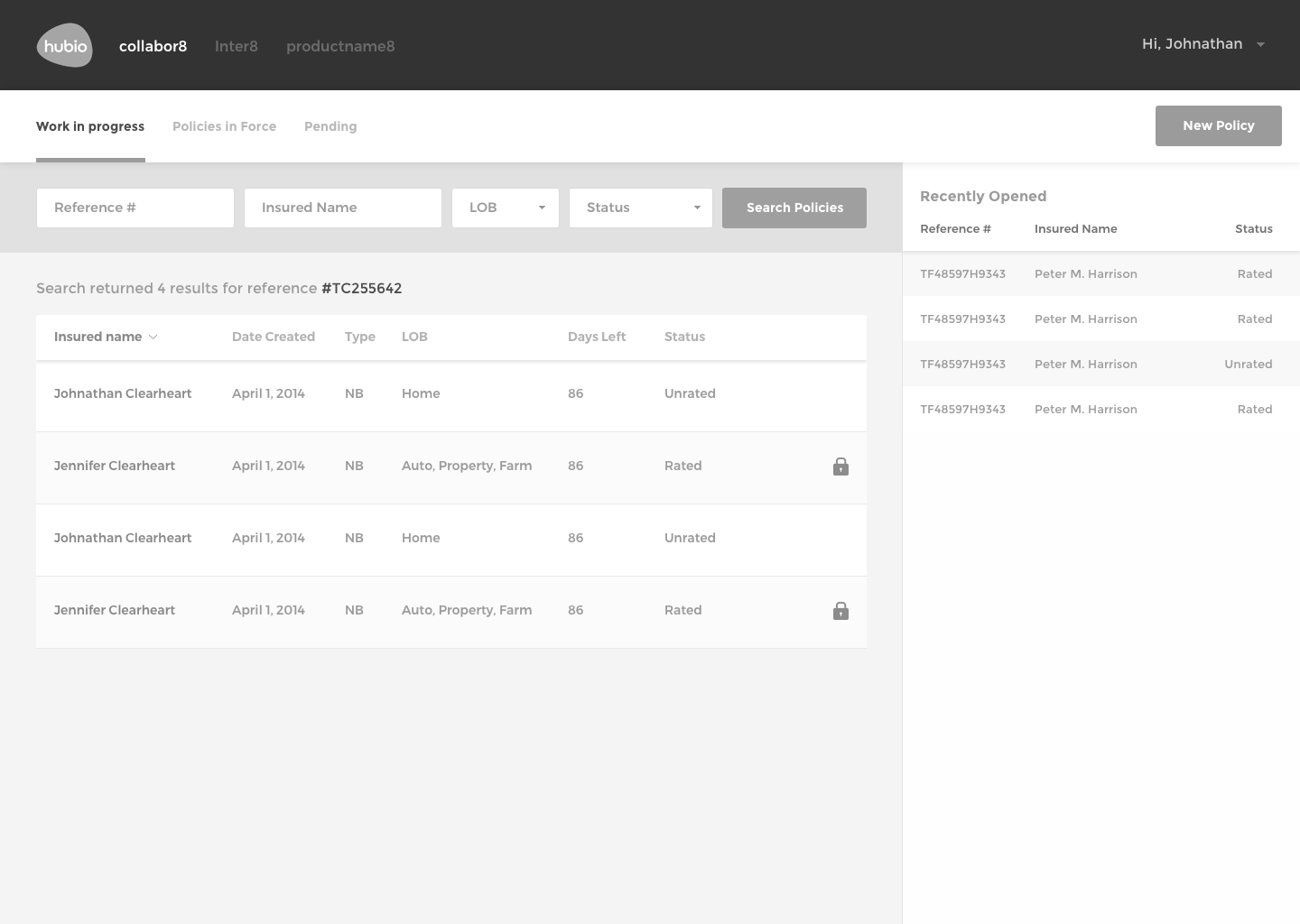
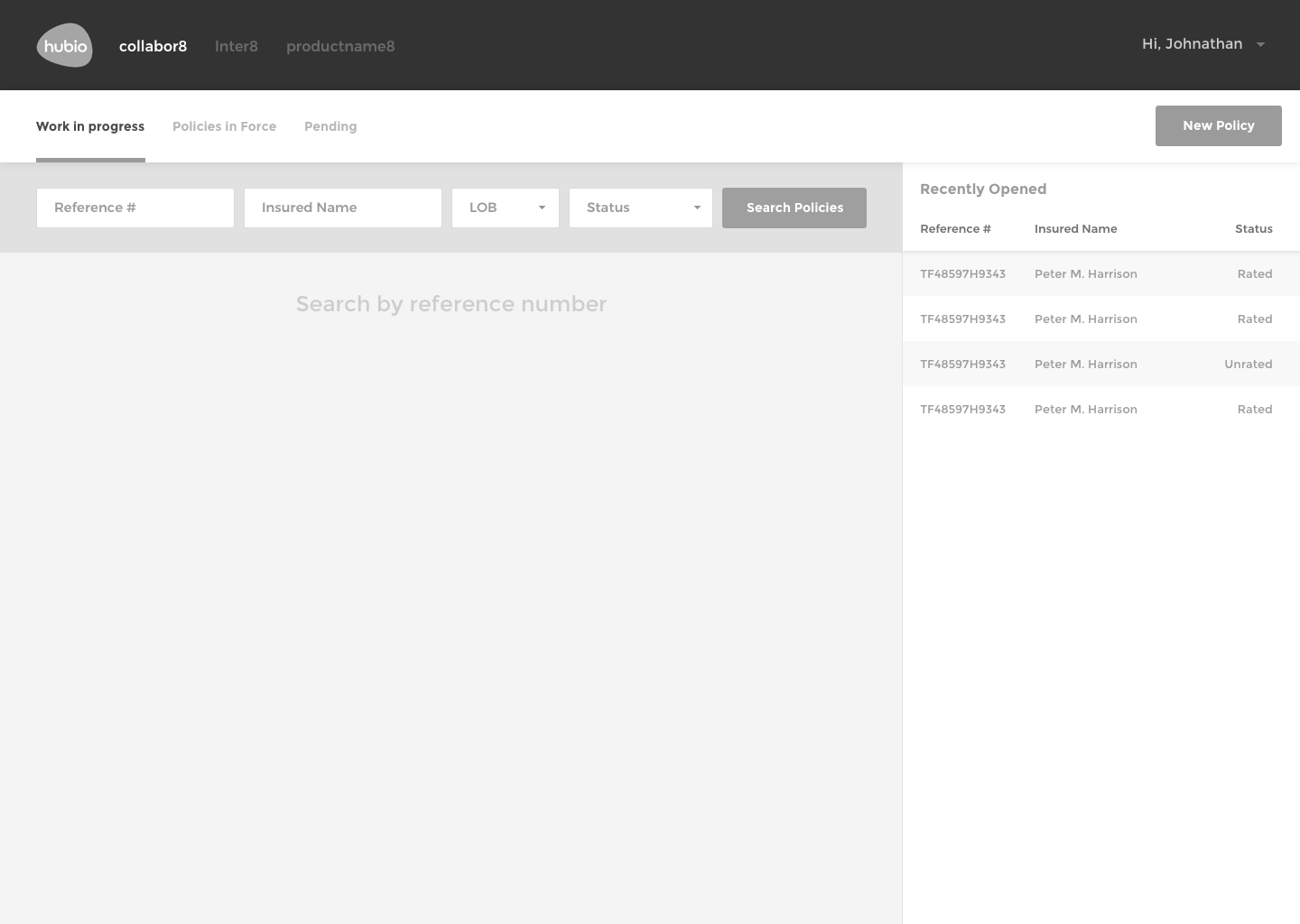
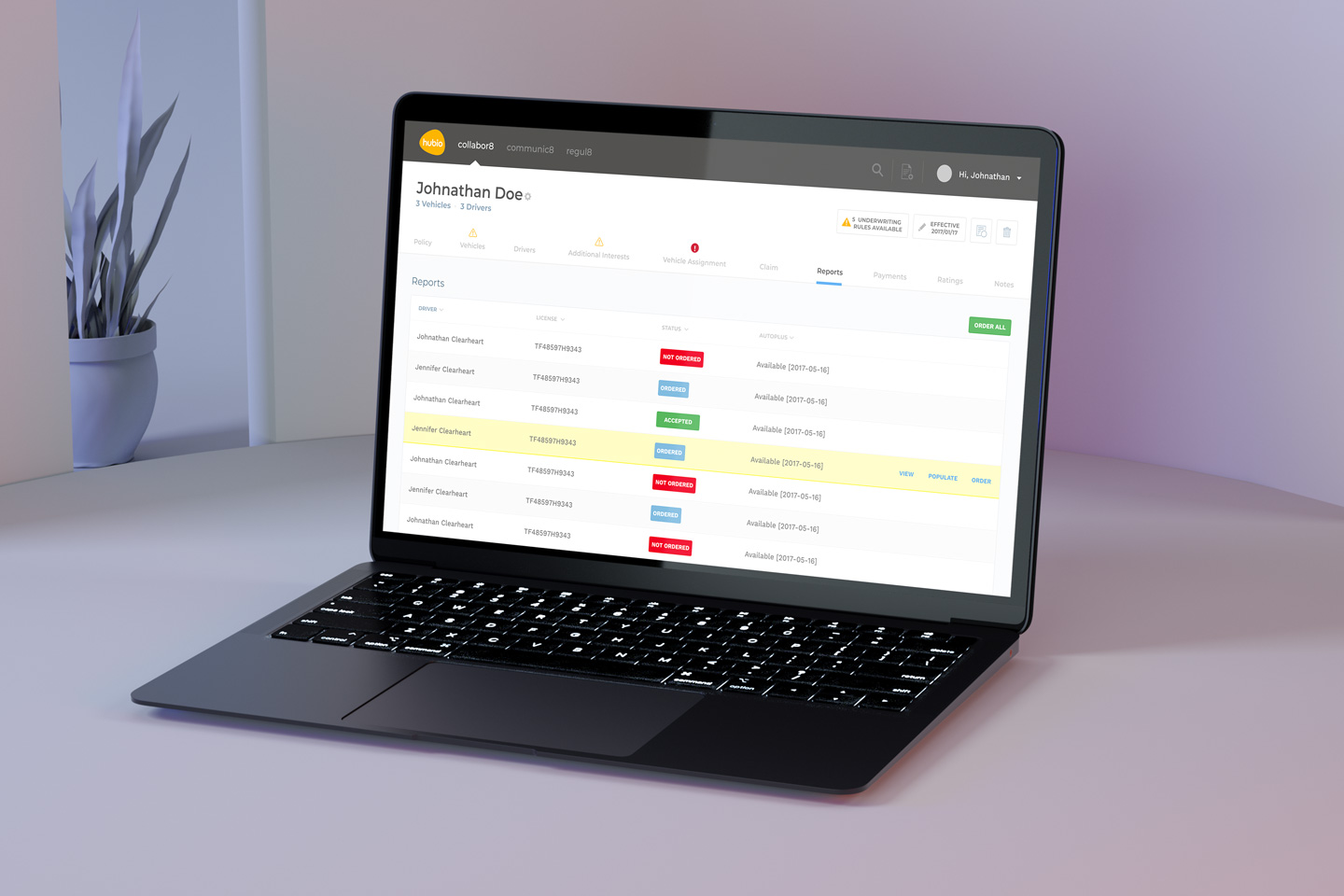
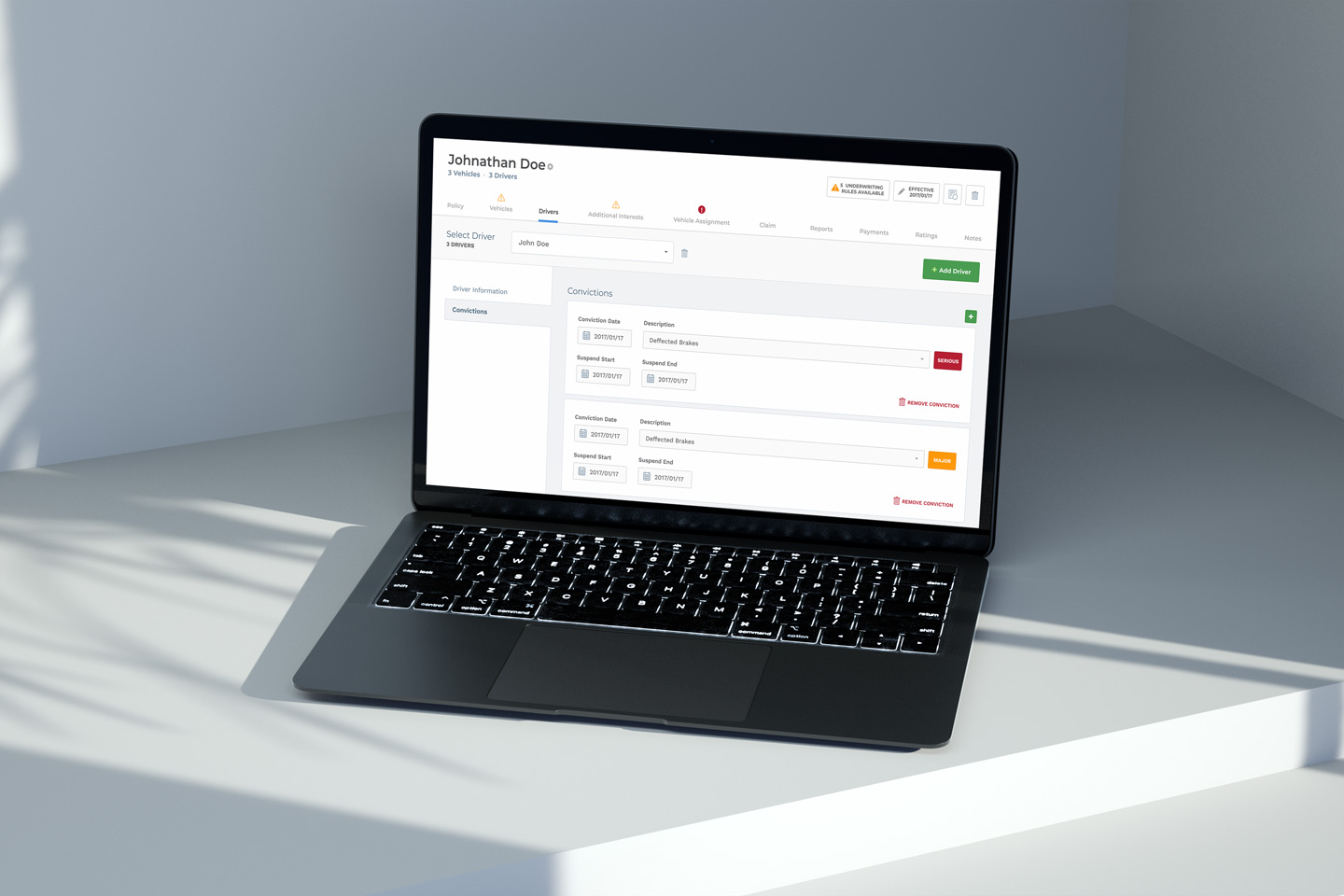
The Solution
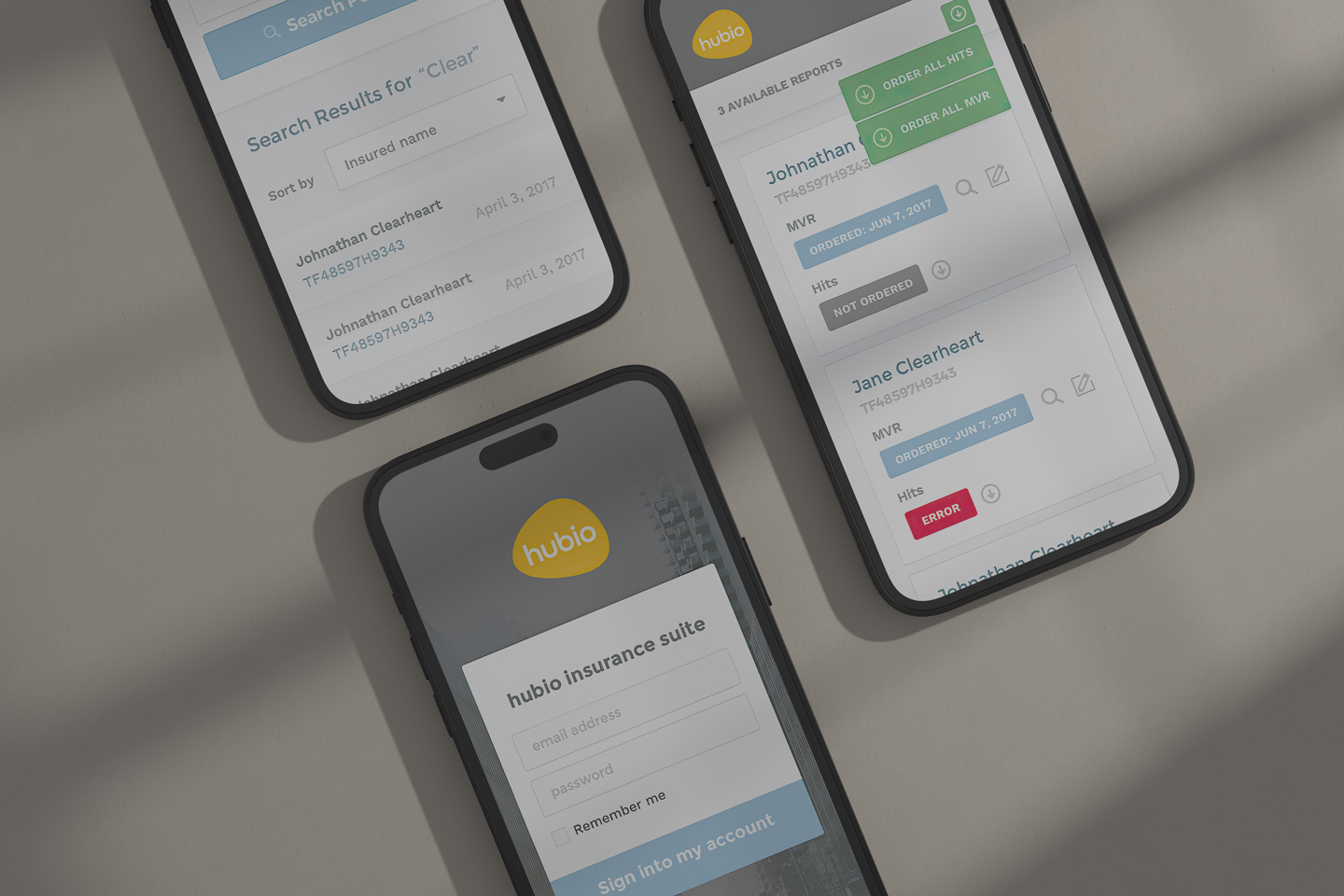
The final design of communic8 includes a web-based user interface for monitoring activity, overseeing interface transactions, error tracking, editing capabilities, and verification processes.
Design Rationale
The design was driven by the need to support a wide range of API formats, ensure end-to-end connectivity, and integrate seamlessly with various systems and standards.
Results and Impact
Better Integration Efficiency
The deployment of Collabor8 led to a 35% improvement in the integration efficiency between insurance companies and third-party providers.
Reduction in Processing Time
The average processing time for claims and underwriting tasks was reduced by 25%, as reported by client feedback.
Increase in Client Acquisition
There was a 20% increase in new client acquisition, attributed to the improved capabilities and efficiencies offered by Collabor8.
Metrics
Operational Efficiency Metrics
Measured by comparing the time taken to complete standard insurance workflows before and after implementing Collabor8.
User Satisfaction Surveys
Conducted at regular intervals post-implementation to gauge the satisfaction levels among different user groups.
Client Acquisition Rates
Monitored through the CRM system, comparing quarterly figures before and after the integration of Collabor8.
Lessons Learned, Challenges & Insights
Integration with Legacy Systems
Integrating Collabor8 with various existing legacy systems posed a significant challenge, requiring custom solutions and additional development time.
Importance of User-Centric Design
The project reinforced the importance of a user-centric approach, especially in understanding the diverse needs of insurance professionals and third-party agents.
Adaptability and Scalability
The experience highlighted the need for solutions like Collabor8 to be both adaptable to different environments and scalable to accommodate growing data and user needs.